Knee Osteonecrosis Specialist

Have you had a sudden onset of knee pain with swelling over the front and inside of the knee? Have you been diagnosed with osteonecrosis of the knee, sometimes called AVN? Osteonecrosis of the knee is a serious condition which requires proper treatment early. Knee osteonecrosis specialist, Dr. James Mazzara provides diagnosis and both surgical and nonsurgical treatment options for patients in Manchester, South Windsor, Enfield, Glastonbury and surrounding Hartford communities who are suffering from osteonecrosis, or “Bone Death.” Contact Dr. Mazzara’s team today!
Osteonecrosis of the Knee
What is osteonecrosis of the knee?
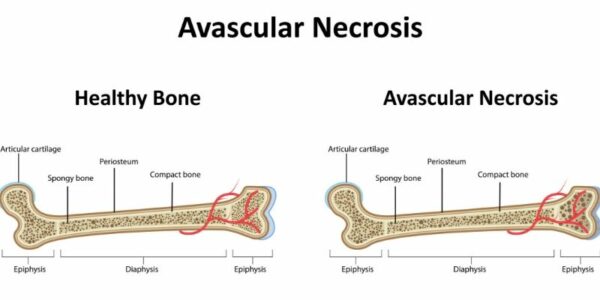
Bone is a living tissue that requires blood and oxygen to survive, much like any other part of the body. Osteonecrosis of the knee occurs when the blood supply to an area of bone is interrupted; this results in the death of that segment of bone. Osteonecrosis is Latin for “bone death” and is referred to as avascular necrosis (AVN), aseptic necrosis, or ischemic necrosis. Bone death caused by osteonecrosis of the knee can result in damage or collapse of surrounding tissue and knee joint. It is important to receive proper early treatment from Dr. James Mazzara, orthopedic knee specialist, serving patients in Manchester, South Windsor, Enfield, Glastonbury and surrounding Hartford communities to prevent permanent joint damage.
What causes avascular necrosis of the knee?
Osteonecrosis of the knee develops when the blood supply to a portion of bone is interrupted and that segment of the bone dies resulting in a series of small continuing fractures which cause the inside and then the outside (cortex) of the bone to collapse. After the bone crumbles, the covering joint cartilage will fail and peel away (delaminate) from the underlying bone. This collapse of bone and failure of the overlying cartilage is usually segmental and only affects one compartment of the knee, usually the medial femoral condyle. The consequences of this bone collapse is profound on the mechanical function of he knee and the infarction of the bone is also painful itself. The cause of osteonecrosis of the knee is unknown. However, doctors have identified risk factors that make patients more likely to develop osteonecrosis.
Risk Factors:
- Oral Corticosteroid Medications: Many conditions are treated with oral steroid medications, including rheumatoid arthritis and asthma. Although it is unknown exactly why these medications can lead to osteonecrosis, research shows there is a connection between the disease and long-term use.
- Prior Knee Injury: A knee injury such as a dislocation or fracture can damage blood vessels and reduce blood flow to the affected bone.
- Medical Conditions: Osteonecrosis of the knee is often associated with certain medical conditions such as lupus, sickle cell anemia, thalassemia, Gaucher’s disease, HIV and obesity.
- Excessive Alcohol Use: A decreased blood supply to the bone can be the result of overconsumption of alcohol which can cause fatty deposits to form in the blood vessels, as well as elevate cortisone levels. Over time, this can result in a decreased blood supply to the bone.
- Transplants: Organ transplants, especially the kidney, is associated with osteonecrosis.
- Gender: Women are three-times more likely to develop osteonecrosis than men.
- Age: Osteonecrosis of the knee can affect anyone, but is most often seen in patients over the age of 60.
- Post arthroscopy osteonecrosis is a rare finding after knee arthroscopic surgery and the causes are unclear. The altered mechanical stresses on the knee after meniscectomy may be a factor. Increased joint pressures on the bone after removal of a portion of the meniscus may lead to small fractures in the underlying bone and cartilage which fail to heal leading to osteonecrosis. The meniscus tear itself may be a cause of the osteonecrosis, usually in patients over 60, and the arthroscopic surgery may just be and intervening but unrelated event.
What are symptoms of knee osteonecrosis?
Avascular necrosis/osteonecrosis develops in stages with the first symptom being pain on one side of the knee, usually the inside or medial side of the knee. The pain may be triggered by a specific activity or minor injury. As the disease progresses, it becomes more difficult to move the knee joint and standing or walking becomes very painful. Other symptoms include:
- Sudden onset of pain
- Swelling over the front and inside of the knee
- Limited range of motion in the knee
- Sensitivity to touch or palpation
- Increased pain at night and with activity
How is Avascular Necrosis Diagnosed?
Osteonecrosis of the knee may take several months to over a year for the disease to progress. It is important to diagnose this disease early, because immediate treatment has shown better patient outcomes. Dr. Mazzara will obtain a medical history and ask about patient symptoms. He will then perform a thorough examination of the knee and look for symptoms specific to AVN. In the early stages of the disease, symptoms may be quite intense and, because routine x-rays are normal, a positive bone scan or MRI may be requested to confirm the diagnosis.
How is Osteonecrosis of the Knee Treated?
The initial treatment for osteonecrosis of the knee is non-surgical, focusing on pain relief and reducing the stress placed on the injured bone. Non-surgical treatment may include:
- Knee Brace: Designed to take pressure off the involved joint surface can aid in healing.
- Crutches: Reduced weight bearing on the affected joint can slow bone damage and help with healing.
- Medications: Anti-inflammatory medications may reduce pain and swelling.
- Exercise: Physical therapy designed to strengthen thigh muscles and reduce stress on the knee joint can be beneficial in bone healing. Often, water exercise is recommended to keep avoid stress on the knee joint.
How to Treat Osteonecrosis with Surgery
If non-surgical treatments fail to alleviate symptoms and associated bone death, surgery may become necessary. Surgical intervention for osteonecrosis of the knee is based on several factors including patient age, extent of damage to the joint and the area of necrosis. For patients in Manchester, South Windsor, Enfield, Glastonbury and surrounding Hartford communities it is important to see Dr. Mazzara, who has extensive experience in treating knee osteonecrosis. Some of the surgical treatments Dr. Mazzara may use are:
- Arthroscopic Debridement and Microfracture: Arthroscopic surgery uses a small camera and small instruments to perform surgery inside the joint. Debridement is when Dr. Mazzara removes loose bits of bone or damaged cartilage from inside the joint space. Microfracture is when small holes are made inside the bone to promote blood flow which can heal the lesion.
- Bone Grafts: Using healthy bone to replace damaged bone. Presently, the bone grafting is a minimally invasive arthroscopic procedure where calcium phosphate can be injected into the avascular segment of the bone encouraging the healing process.
- Osteotomy: A procedure that involves cutting the bone and changing the realignment to relieve stress on the bone or joint.
- Partial joint replacement: This is reserved for knees where the cartilage is otherwise normal and the knee is well aligned but there is a compartment of the knee where the osteonecrosis has resulted in bone and cartilage dame that cannot be treated by other means.
- Total Joint Replacement: In this procedure the entire knee is replaced. All compartments of the knee are actually resurfaced usually because, in addition to the osteonecrosis, the other parts of the knee are also arthritic.
- Arthroscopic decompression: This is a minimally invasive procedure where the infarcted of avascular segment of the bone is drilled to reduce bone pressures and encourage the healing of the bone by creating new channels into which new circulation will enter, encouraging the body to heal itself. It is a way to jump start the body’s own healing response. Presently, we would also inject calcium phosphate into the bone making it stronger as well. This injection of calcium phosphate is called a “subchondroplasty”.
Patients who have osteonecrosis of the knee are urged to seek medical care early. If you have questions about knee osteonecrosis and the correct treatment for you, please contact the orthopedic offices of Dr. James Mazzara, knee specialist in Manchester, South Windsor, Enfield, Glastonbury and surrounding Hartford communities.